The ward at Clinique Kinoise in Kinshasa, Democratic Republic of the Congo (DRC) buzzes quietly with activity. As Kinshasa’s primary referral center for severe mpox cases, the 42-bed facility serves two purposes—providing maternity care and mpox isolation and treatment. The facility offers general consultations, maternal and newborn health care, and specialized diagnostic services, including testing for malaria, HIV, and mpox.
A young mother sits on the edge of one of the beds, gently rocking her newborn as the baby’s tiny fingers curl around hers; she has been admitted with a presumptive mpox diagnosis after presenting to the facility with characteristic rashes. Additionally, she does not yet know her HIV status—a critical gap, considering that people living with undiagnosed HIV are at higher risk for severe mpox illness and complications. In the next bed, separated by a thin curtain, another woman rests after mpox treatment.
Down the hall, a nurse checks on a mother referred from a rural clinic far outside the city. In a single visit, women, mothers, and their babies come with multiple health issues, but the system isn’t yet designed to identify and address them at once.
“You see the weight women carry. They do not come for one thing. They come with everything.”— Dr. Albert Komba, SAFEStart+ Project Director
This is the everyday reality Dr. Albert Komba encountered during his first visit to DRC as project director of SAFEStart+, an initiative funded and supported by Unitaid to accelerate demand and adoption of integrated approaches to eliminate vertical transmission of HIV, syphilis, hepatitis B, Chagas disease, and mpox across nine countries.
He had joined PATH just one month earlier.
“I have spent my career in clinics. In villages. On the roads. Going where people are,” he said. “You see the weight women carry. They do not come for one thing. They come with everything."
During the visit, Dr. Komba, with hosts—the PATH DRC SAFEStart+ team and government health administrators—toured Clinique Kinoise, one of the few specialized centers in Kinshasa that admits, manages, and monitors mpox cases.
In a country that consistently reports Africa’s highest number of mpox infections, facilities like this are on the front lines. The site visit team suited up in full personal protective equipment, including caps, masks, gowns, double gloves, and shoe covers, before moving carefully through the ward to speak with clients and staff.
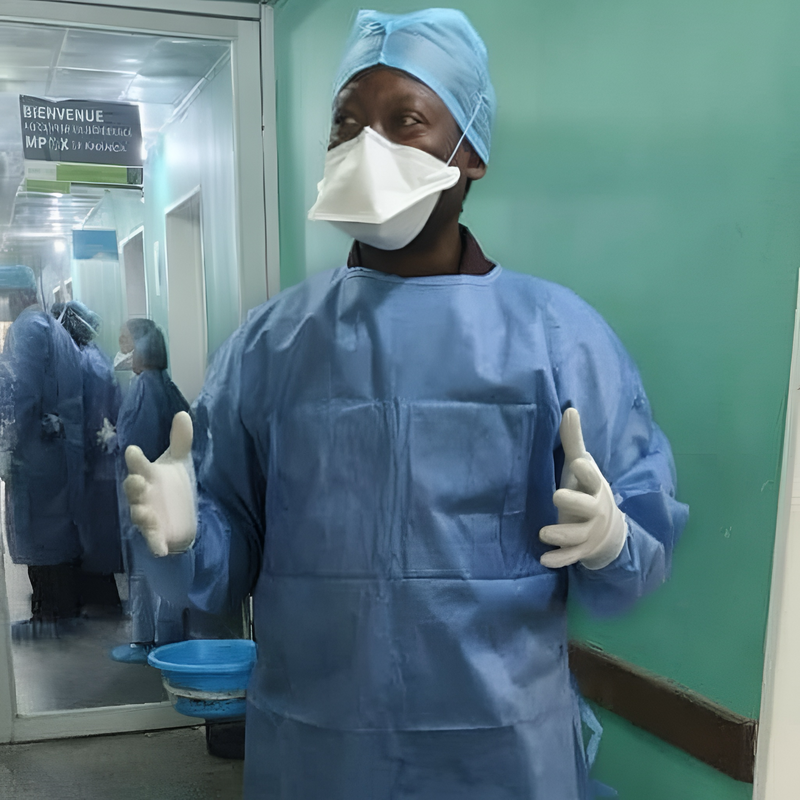
Dr. Albert Komba, SAFEStart+ project director, stands in full personal protective gear inside the mpox isolation ward at Clinique Kinoise in Kinshasa, DRC. Photo: PATH/Deborah Bongonda.
One encounter stayed with Dr. Komba. A newborn, just a few weeks old, was being treated for mpox. The child had an extensive rash that spread to affect their eyes. It was a stark reminder of how diseases like mpox, as well as HIV, syphilis, and hepatitis B, can spread to a baby during pregnancy, childbirth, or breastfeeding—also called vertical transmission.
In a country still healing from Ebola outbreaks, vertical transmission can make care more complicated, especially when managing multiple diseases.
It is precisely this overlap that SAFEStart+ is designed to address by integrating screening, treatment, and prevention for multiple diseases into the daily flow of primary health care services. This includes introducing and expanding access to new diagnostics that can detect multiple diseases with a single test and reinforcing antenatal (ANC) and postnatal care (PNC) when it matters most.
A diverse landscape of care
The DRC’s health system is large and diverse. HIV testing is now routine in many places and nearly all pregnant women attend at least one ANC visit—but gaps still exist. Syphilis screening reaches fewer than half of pregnant women.
While the DRC has included hepatitis B birth dose in its routine childhood immunization schedule since 2007, the country has not yet fully implemented a universal birth-dose policy despite World Health Organization (WHO) recommendations that the vaccine be administered within 24 hours of life to prevent vertical transmission. And in a country where more than 6.9 million people have been displaced by conflict, follow-up care can be challenging to maintain.
Just as gaps persist across routine maternal and HIV/hepatitis/syphilis services, mpox exposes and deepens these same weaknesses. Where coverage, continuity of care, and reach are already uneven, particularly in remote areas, the lack of decentralized approaches for mpox screening limit early detection and timely response.
Despite a growing number of commercial tests, nearly half of mpox diagnostics remain research‑use only or lack regulatory clarity and no independently validated rapid diagnostic tests are yet available. As a result, mpox diagnostic services continue to be centralized at laboratories with long turnaround times, allowing outbreaks to spread undetected in hard‑to‑reach areas.
“These efforts show what is possible. Now we need to connect them. Make them work together.”— DRC Ministry of Health official
Yet progress is real.
In June 2025, President Félix Tshisekedi launched the Presidential Initiative to End Pediatric AIDS, which aims for better testing and treatment for mothers and children. Two labs in Kinshasa received international accreditation in March—the first in the country—thanks to years of support from the US Centers for Disease Control and Prevention and the US President's Emergency Plan for AIDS Relief.
“These efforts show what is possible,” a DRC Ministry of Health official shared. “Now we need to connect them. Make them work together.”

A health care provider in Vietnam counsels a woman during an antenatal care visit on the importance of knowing one’s syphilis, HIV, and hepatitis B status to prevent potential onward transmission. Photo: PATH/Phan Thanh Tuyen.
A catalytic investment building on existing strengths
That’s where SAFEStart+ comes in: not to replace what is there but to enhance current delivery platforms and systems by expanding proven approaches and generating evidence to drive adoption and scale of innovations, with communities and countries leading the charge.
This four-year, $22 million Unitaid-funded project is led by PATH, the International Community of Women Living with HIV Eastern Africa, and the World Hepatitis Alliance, along with other technical and research partners and country-level implementers.
“SAFEStart+ is a catalytic investment. We are not creating new systems; we are working with communities and supporting countries to improve the existing ones.”— Dr. Albert Komba, SAFEStart+ Project Director
The project’s goal is simple: to prevent vertical transmission so diseases end with one generation, rather than spreading to the next. SAFEStart+ aims to approach this goal through five clear parts:
- Country-led demand and scale of models to eliminate vertical transmission (EVT): Women are at the heart of the initiative. Through assessments, human-centered design, and ongoing quality improvement, the project will work with women and other people with lived experience, community-led organizations, and governments to co-design and roll out integrated models that suit women’s lives—delivering integrated care that is timely, respectful, and practical. This will be complemented by systems improvements to ensure uninterrupted availability of needed commodities, trained and supported health care providers, and strengthened access to accurate and timely data for enhanced client care management and decision-making. Community advisory boards and national technical working groups will oversee every step.
- Targeted learning: The project will drive programmatic monitoring and evaluation, targeted implementation science, and modeling, and share learnings on people-centered and efficient strategies as well as approaches and tools to enhance EVT access and uptake. Costs, quality, and outcomes will be tracked to identify what works and why.
- Strategic market shaping for EVT products: Market shaping efforts will ensure diagnostics and medicines for treatment and prevention remain affordable and accessible. Supply chains will be reinforced. Regulatory processes will accelerate.
- Country adoption and financing of EVT programs: SAFEStart+ is jointly designed with countries from the outset. Governments and community partners will develop and test solutions, enabling access to evidence and investment cases to continue funding and sustaining integrated programs long after the project concludes.
- Integration of mpox into EVT platforms: In the DRC, the project will accelerate WHO-recommended methods for mpox testing and care among pregnant women and their partners, newborns, and young infants within existing EVT platforms.
The project provides tiered technical support to nine countries across Africa, Asia, and Latin America, including the DRC, with innovations and lessons from these geographies shared with ten additional peer-learning countries to enhance their existing EVT platforms. WHO and the Pan-American Health Organization will further facilitate regional knowledge sharing and help shape markets to ensure innovative approaches and tools reach a wider audience.
In the DRC, the project will not start from scratch.
It will build upon the national triple elimination plan for HIV, syphilis, and hepatitis B by leveraging routine ANC and PNC for epidemic preparedness and response. SAFEStart+ will integrate mpox screening and care for pregnant women during ANC and PNC—enabling women to be screened for multiple diseases in just one visit—and coordinate with the mpox response and other health teams to reach women, whether they are pregnant or postpartum, whether they are in Kinshasa or elsewhere.
Small grants will support local community networks to reach families of pregnant women, encouraging male partners and children to get involved, and improve training to help health care workers deliver care with confidence.

In a clinic waiting area, a health provider talks to mothers as they hold their infants. These spaces are the ones SAFEStart+ aims to strengthen to help protect the next generation from preventable diseases. Photo: PATH.
A future vision in motion
In the coming months, SAFEStart+ will expand across the DRC and eight other countries. Health care workers will be trained; clinics will be stocked with essential equipment and supplies; multi-disease testing, treatment, and prevention will become part of standard ANC and PNC care; and community networks will lead outreach to mothers who might otherwise be missed.
Looking ahead: we envision that, by 2030, babies born in these nine countries will no longer suffer from preventable diseases. Across all locations, SAFEStart+ expects to prevent 47,000 infections and save 179,000 years of healthy life. Each number represents a child growing up healthy and a family staying safe.
When this approach takes hold, the experience will change.
A mother walks into a clinic, either for antenatal care, expecting to give birth, or having just given birth. During that visit, she learns her HIV, syphilis, hepatitis B, Chagas, and mpox status. If any test is positive, she will be initiated on treatment and/or preventive therapy immediately, and her partner will be offered testing. Her newborn is checked at birth and given a hepatitis B vaccine within the first 24 hours. Her medical records follow her wherever she goes.
Dr. Komba summed it up simply: “SAFEStart+ is a catalytic investment. We are not creating new systems; we are working with communities and supporting countries to improve the existing ones. That way, every woman knows her status, and every child can be born free of these diseases.”
This is what integrated, people-centered care looks like. This is what SAFEStart+ aims to achieve.



