For a long time, health care delivery in India—and indeed, in many other low- and middle-income countries—has been done via ‘vertical disease programmes’. In other words, the National Tuberculosis (TB) Elimination Programme provides services for TB, the National AIDS Control Programme provides services for people living with HIV, and so on. Whilst this approach has led to many impressive gains in disease control, it has also created systemic weaknesses on three significant planes:
- First, a disease-focused strategy tends to make the entire health care system disease-centric rather than patient-centric. Under such a system, if the same patient has TB and diabetes, he or she is required to have samples drawn at different clinics (often located far from each other) and to be managed by different health care providers, who are unable to view and correlate the diagnostic results from different labs. As a result, care providers are unable to treat the patient as a whole.
- Second, it leads to duplication of infrastructure, equipment, and personnel, and so to underutilisation and wastage.
- Third, and perhaps most alarming, this approach leads to gaps in outbreak management—a disease-focused health care system has limited capacity to carry out comprehensive surveillance, prepare for outbreaks, and mount timely human and infrastructural responses when one occurs.
A further gap in the current diagnostic landscape is that there are no systems for coordination between health-focused and other related departments, such as food, water, climate, and veterinary sciences. These have not traditionally been seen as partners for human health but are rapidly becoming more relevant for all health outcomes, especially for areas like antimicrobial resistance and environmental surveillance.
One-health approach, integrated labs, and block units
Driven by an increased understanding of the vulnerabilities of siloed health care systems and by the growing global shift towards a ‘one-health approach’, the government of India has taken a number of steps to bring the country closer to systemic integration of various health services and to universal health coverage.
In 2021, the government launched the Pradhan Mantri Ayushman Bharat Health Infrastructure Mission to develop the capacities of health systems and institutions across the continuum of care and prepare health systems to respond effectively to current and future pandemics.
Critically, the Mission also aims to build an information technology–enabled disease surveillance system by developing a network of laboratories at block, district, regional, and national levels and strengthening health units at point of entry for effectively detecting, investigating, preventing, and combating public health emergencies. Specifically, the network would be made up of Integrated Public Health Laboratories (IPHLs) and Block Public Health Units (BPHUs).
The classification of IPHL extends to any laboratory which provides comprehensive lab services all under one roof, including diagnostic as well as surveillance services, and which participates in an interconnected data management system. BPHUs are block-level facilities designed to serve remote areas and unreached populations. They act as referral hubs for peripheral facilities, namely Ayushman Bharat—Health & Wellness Centres and community and primary health care centres. In turn, IPHLs will be hubs for BPHUs. Labs in an integrated laboratory model will talk to each other, as well as with systems and stakeholders in both upstream and downstream channels of the health system.
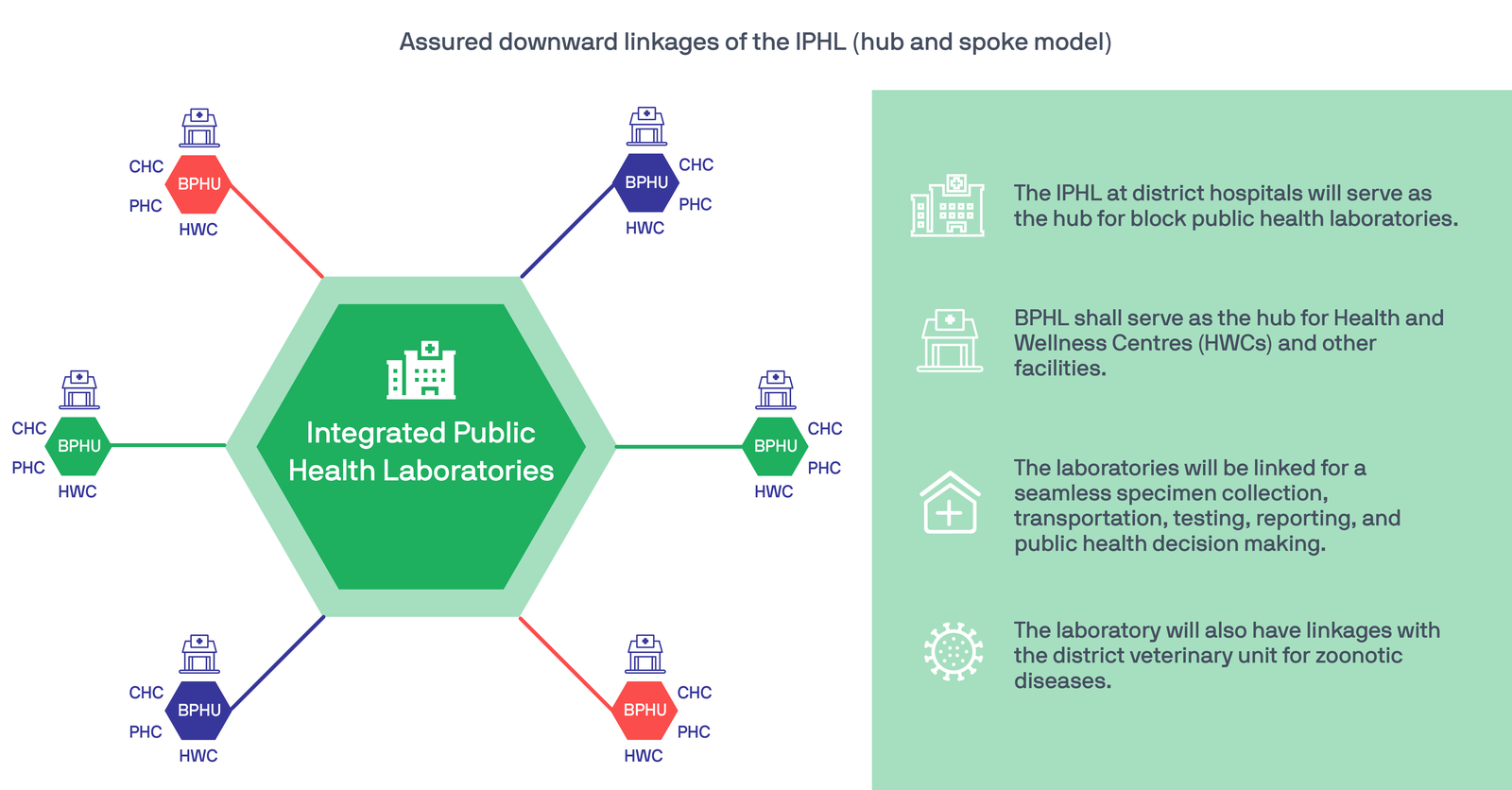
The establishment of these labs at the block and district levels will:
- Increase efficiency, reduce redundancy, improve service, and better prepare laboratories for emerging disease threats.
- Alleviate the country’s disease burden by providing rapid, reliable, and accurate test results for optimal patient care and health outcomes.
- Shift focus from curative care to preventive care.
- Reduce out-of-pocket expenditure on diagnostics.
- Reduce the abrupt use of drugs, which in turn would reduce drug resistance.
In addition to optimal health care outcomes, this systemic approach can lead to best-in-class surveillance for all diseases and future pandemics for 1.4 billion Indians. IPHLs are an appropriate platform for the one-health approach, providing much-needed coordination between health and other departments, including ones for veterinary sciences, agriculture, and the environment and climate change.
PATH is catalysing the change
Integrated labs are the future of accessible and affordable diagnostics—crafted to take India closer to universal health coverage. Complete with disease, function, and data integration, as well as downward and upward linkages, this network of integrated labs has the potential to transform diagnostics and surveillance in the country.
PATH has begun the work in this direction. With decades of expertise in advancing diagnostics and surveillance, we are providing technical assistance, guided by a human-centred design approach, to several states across the country in the creation of lab networks that can provide affordable diagnostics to the community and that are surveillance-ready for disease outbreaks. We also support the National Health Systems Resource Centre in implementation and innovation.
PATH also looks forward to supporting the states through the following activities:
- Planning integrated diagnostics labs at the district and block levels by selecting implementation geographies and facilities and providing technical assistance to block-, district-, and facility-level institutions for focussed activities, like creation of a technical support unit, customisation of IPHL and BPHU layout designs, and development of an implementation roadmap and project management plan.
- Providing technical and operational support for fast-tracked and collaborative implementation of IPHLs through infrastructure development, human resource capacity-building, laboratory management information system, systemic integration, process improvements, and transition planning.
- Providing technical and operational assistance to build and demonstrate long-term surveillance and intersectoral coordination by expanding public health system capacity through blueprints, standard operating procedures, and Centres of Excellence.
Vision for strengthened health systems
With an eye on sustainability, PATH designs the interventions to enhance the capacity of various stakeholders in the government health care system. We will play a catalytic role in periodic review of the systems instituted for identifying gaps and recommending corrective actions. Effective knowledge transfer to the relevant government stakeholders at various levels will ensure that requisite capacity is built within the government health machinery for scaling up the interventions.



