In 2021, while navigating the second year of the COVID-19 pandemic, the global malaria community continued advancing its mission to eliminate malaria. Along the way, history was made and pictures were taken. Here are ten that show what PATH Malaria and partners were up to in 2021.
1. Using mosquitoes' sweet tooth against them

An ATSB monitor installs a bait station on a household in an intervention cluster in Kaoma District, Western Province, Zambia. Photo: PATH/Erica Orange.
In 2021, PATH continued its work evaluating attractive targeted sugar baits (ATSBs). Hung on the outside walls of households, ATSBs aim to address outdoor malaria transmission by uniquely capitalizing on the sugar-feeding behavior of mosquitoes; they attract mosquitoes with a sugar meal that includes a toxicant specifically lethal to mosquitoes. ATSBs may also be a particularly important vector control tool in the context of managing insecticide resistance, as other ingestion toxicants can be rotated.
From February to June, PATH, in partnership with the Ministry of Health, Innovative Vector Control Consortium (IVCC), the Center for Applied Malaria Research and Evaluation at Tulane University, and the Macha Research Trust, deployed sugar baits containing dye rather than toxin as part of a study that measured the feeding rate of recaptured mosquitoes and compared mosquitoes caught in clusters with two baits installed per structure versus clusters with three.
The results from the study informed the ATSB deployment strategy for the ATSB trial launched in November 2021 in 70 clusters in three districts in Western Province, Zambia. Trial activities include the deployment of nearly 40,000 ATSBs, the enrollment of over 2,000 children in a seasonal cohort study, and monthly entomological monitoring. The trial team conducted intensive community sensitization to prepare communities for the two-year trial.
2. Proactively identifying and treating malaria

Community health workers Gertrude Banda (left in orange shirt) and Florid Mufwali (right in orange shirt) collect data during a baseline survey for the ProACT study in Chadiza District, Eastern Province, Zambia. Photo: PATH/Elizabeth Chiyende.
In April and May, PAMO Plus, a project funded by the US President’s Malaria Initiative and implemented by PATH, conducted a baseline survey in Chadiza District in Zambia’s Eastern Province to collect data on malaria prevalence. This represented the initial steps of the ProACT study, a three-year study that investigates if proactive community case management of malaria by community health workers—conducted by visiting every household in the community weekly to detect people with malaria symptoms, offer diagnosis, and treat those who test positive—will lead to a greater reduction in parasite prevalence and case incidence compared to the existing, passive form of community case management. These baseline data will be compared with endline data to look for changes over time and to compare intervention and control arms.
3. Achieving regulatory approval for a new diagnostic test

Huyen Nguyen of PATH (seated on left) observes health care staff in Binh Phuoc Province, Vietnam, after a training session on G6PD testing to assess staff proficiency and competency. Photo: PATH/Spike Nowak.
It was an important year for SD BIOSENSOR’s STANDARD™ G6PD Test. In May, the diagnostic test—the first point-of-care test for glucose-6-phosphate dehydrogenase (G6PD) deficiency that can support safe access to the currently available drugs that treat Plasmodium vivax malaria—received regulatory approval from the Australian Therapeutic Goods Administration (TGA).
The approval by the TGA certifies that the test is appropriate for use and meets rigorous quality standards; furthermore, it expands access of malaria treatment and decision-making to locations where people initially seek health care—at primary health care facilities, dispensaries, and possibly even through trained community-level health care workers.
The PATH Diagnostics team and SD BIOSENSOR supported the advancement of the test through product development and clinical evidence generation for submission to the TGA and the World Health Organization’s Prequalification of In Vitro Diagnostics Programme, where it is currently under review. The PATH Market Dynamics team is supporting the introduction of the test into routine health settings.
4. Sequencing COVID-19 infections and mapping variants
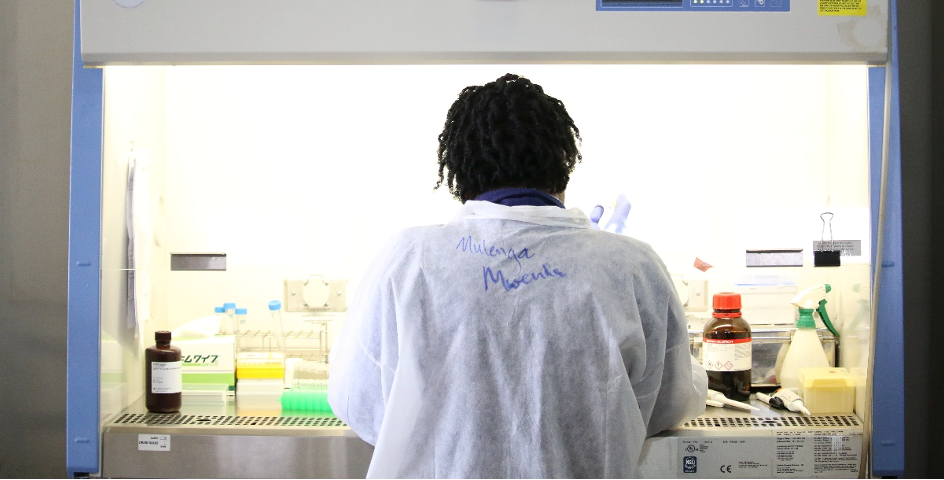
Mulenga Mwenda-Chimfwembe, a laboratory scientist at PATH, sequences SARS-CoV-2 samples. Photo: PATH/Mirriam Chimba.
In May 2021, when PATH’s lab team in Lusaka, Zambia, identified the Delta variant of SARS-CoV-2 in the country, it marked yet another stage of the evolution of the team’s work. Prior to May 2020, the lab had been focused on the genomic sequencing of malaria parasites. However, when the first wave of COVID-19 infections hit Zambia, the team began applying its expertise to SARS-CoV-2.
Since then, in partnership with the University of Zambia’s School of Veterinary Medicine, the team has sequenced more than 1,000 infections and mapped the rise and fall of different variants. The first African team to identify the Beta variant outside South Africa, the team has now received funding to expand its focus from generating data to strengthening sequencing skills within the Zambian government.
The hope is to build capacity in this important area to enable the government to better target and coordinate sequencing for maximum impact. While the PATH sequencing team will continue to support SARS-CoV-2 work, they are also continuing their work on genotyping parasites to look for molecular markers of resistance to common malaria treatments.
5. Implementing additional response measures
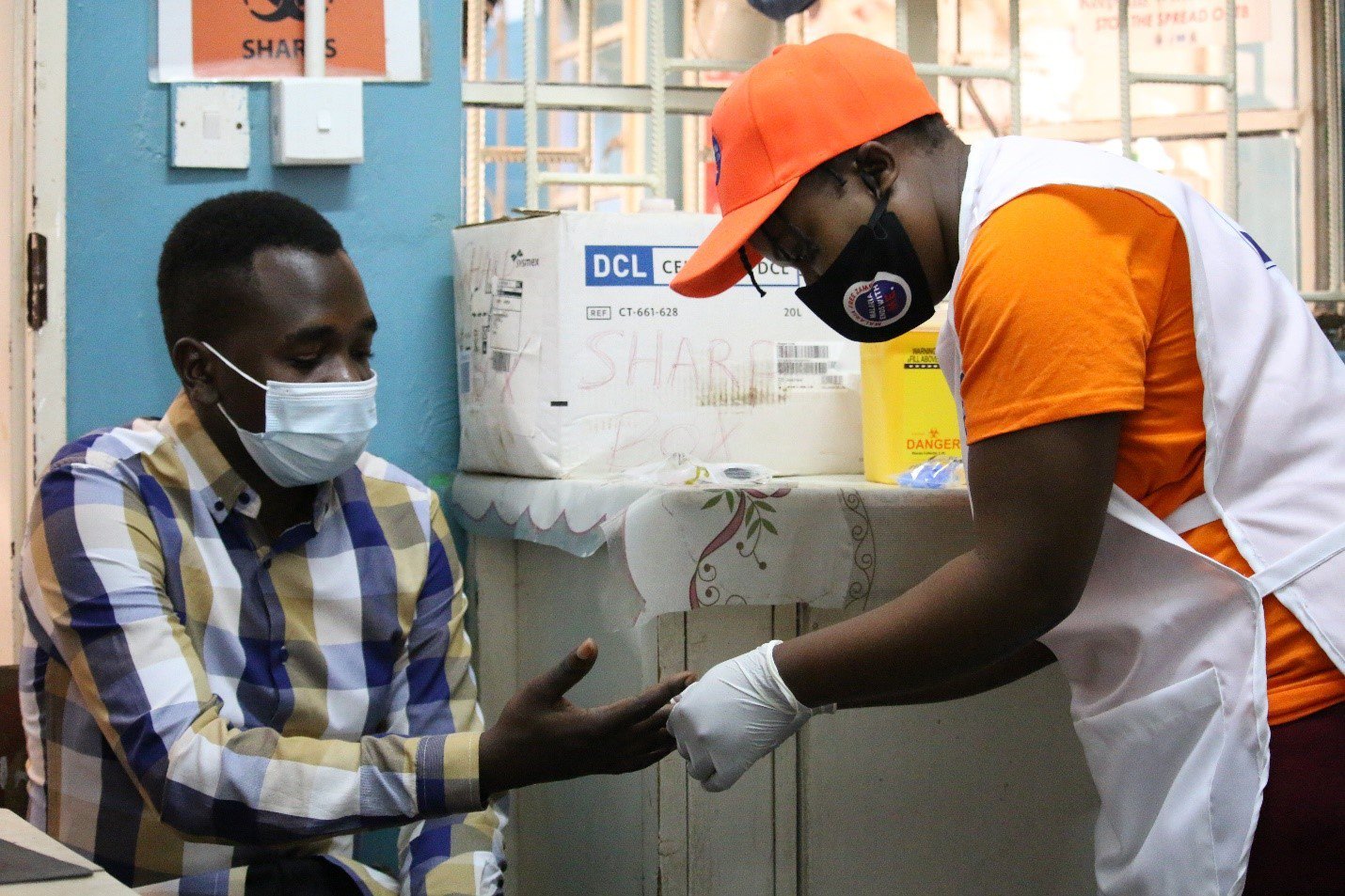
Community health worker Bernadette Chilufya (right) conducts a routine diagnostic test on patient Christopher Chewe at Nakambala Health Facility in Mazabuka, Zambia, during malaria case investigation trainings. Photo: PATH/Chilowekwa Shike.
In Zambia, in areas of very low malaria transmission, standard practice for handling suspected cases has involved prompt testing, treatment if malaria is confirmed, and then a follow-up to track and clear the infection at the patient’s and neighbors’ homes.
In September, Zambia began implementing malaria case investigation (MCI), an intervention that goes beyond the existing approach with a confirmed malaria case triggering a prompt and comprehensive response that includes collecting dried blood spots for laboratory investigation, identifying and addressing potential mosquito breeding sites, and performing reactive indoor spraying and/or gap-filling with bed nets as needed. MCI is modeled on strategies that have seen success in other countries, particularly China’s 1-3-7 approach (case reporting within one day after diagnosis, case investigation within three days, and foci investigation and action within seven days).
6. Making history with the world’s first malaria vaccine
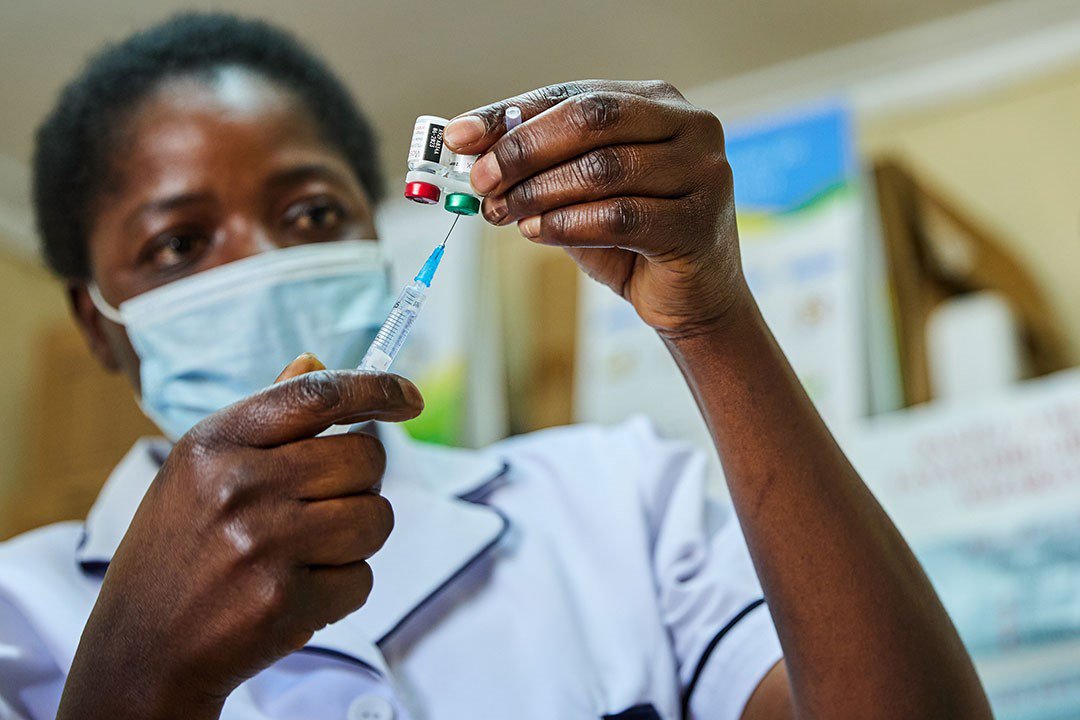
Nurse Janet Wanyama prepares to vaccinate a child with the RTS,S/AS01 malaria vaccine at Malava County Hospital in Kakamega, Kenya. Photo: Gavi/2021/White Rhino Films-Lameck Orina.
In October, history was made as RTS,S/AS01 (RTS,S) became the first malaria vaccine and first vaccine to combat a human parasite to be recommended by the World Health Organization (WHO). The recommendation is for the vaccine to be used in children at risk in areas of moderate to high Plasmodium falciparum malaria transmission, primarily in sub-Saharan Africa.
Shortly after the recommendation, the board of Gavi, the Vaccine Alliance approved a malaria vaccination program to support the broader rollout of RTS,S. The program will provide funding for vaccine procurement, technical assistance for vaccine introduction, and other activities that will enable interested, Gavi-eligible countries to apply for support to introduce the vaccine.
PATH has been involved in the development and introduction of this vaccine since 2001, when a partnership with the vaccine’s developer and manufacturer, GSK, was established. In 2017, PATH entered into a collaboration with WHO, GSK, and the ministries of health in Ghana, Kenya, and Malawi to support pilot implementation, which began in 2019. Now, PATH is working with partners and other stakeholders to help ensure sufficient supply of the vaccine will be available to meet the anticipated demand over the coming years.
7. Ensuring a timely and efficient response to malaria

(L to R) Trad Hatton (PATH), Nicolas de Borman (Bluesquare), Hana Bilak (PATH), Health Minister Jean-Jacques Mbungani, and Grégoire Lurton (Bluesquare) at a DRC Ministry meeting where the EOC-Malaria team presented data visualization dashboards.
Emergency operations centers (EOCs) are an important part of how countries can identify and respond to outbreaks in a timely way. EOCs coordinate analysis and use of data to enable outbreak prevention and ensure public health emergencies are adequately dealt with and that response is promptly organized.
After integrating malaria into the scope of EOCs in Senegal, The Gambia, and the Democratic Republic of the Congo (DRC) in 2020, the EOC-Malaria project (a consortium of PATH and Bluesquare funded by the Bill & Melinda Gates Foundation) continued its work in those countries in 2021 and in October launched a new investment in Vietnam in partnership with Population Services International. These projects aim to support ministers of health to respond to COVID-19 and mitigate its impact on malaria and to explore how EOCs can be leveraged to strengthen the use of data to support malaria elimination and burden reduction.
8. Identifying and reaching those at high risk

PATH and Saraya District staff walk to gold mining sites in Saraya District, Senegal, to conduct a malaria survey among gold miners in October 2021. Photo: PATH/Henry Ntuku.
To eliminate malaria, it is important to identify populations with a higher risk of infection and determine the optimal package of interventions for those specific populations. In Senegal, PATH, the national malaria program (Programme National de Lutte contre le Paludisme, or PNLP), and the University of California San Francisco (UCSF) reviewed available data and identified three potential high-risk populations: nomadic pastoralists, gold miners, and Koranic school students. A study was then conducted in October (and is ongoing through January 2022) by PATH, PNLP, and UCSF in the districts of Ranérou, Kaolack, and Saraya, in areas often not accessible by car or motorbike, to understand their exposure profile, identify malaria risk factors, and target them with tailored interventions.
9. Visualizing entomologic data
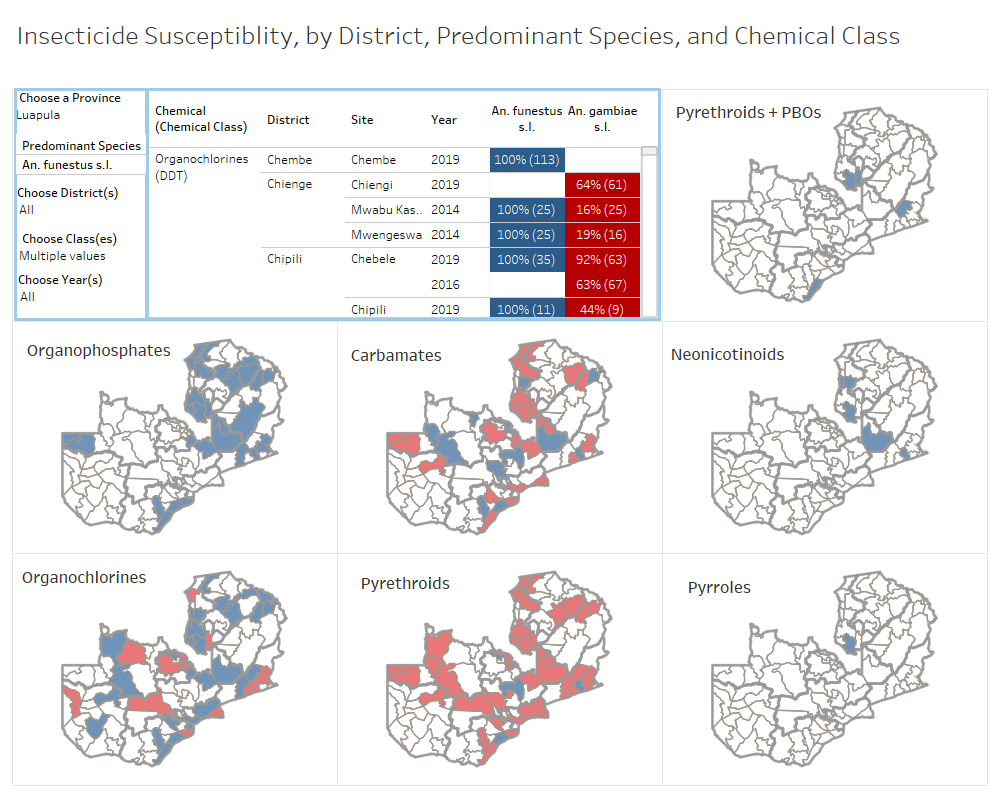
Insecticide resistance data across multiple partners are analyzed and visualized to guide decisions on the selection and rotation of insecticides for indoor residual spraying and insecticide-treated net campaigns in Zambia. Photo: PATH.
In December, PATH supported the National Malaria Elimination Programme in Zambia with visualizations like the one above to integrate entomological data from multiple partners to inform the selection and rotation of insecticides for indoor residual spraying and insecticide-treated net campaigns in Zambia.
Through the US President’s Malaria Initiative (PMI) VectorLink Project, PATH is supporting national malaria programs in ten countries (Burkina Faso, Cote d’Ivoire, Ethiopia, Liberia, Madagascar, Malawi, Mali, Nigeria, Sierra Leone, and Zambia) to evaluate the impact of vector control interventions and guide national vector control decision-making. The team combines local routine data sources and malaria case incidence, residual spraying and bed net program data, entomology indicators, and climate data to create interactive visualizations and conduct statistical analyses. The results are then used by the national programs and PMI to assess the impact of these lifesaving interventions and inform national vector control program decisions.
To learn more about PATH’s work under VectorLink, read the project’s program brief, case studies, and best practices guide for integrating and visualizing vector control data for decision-making.
10. Demonstrating the potential impact of new types of bed nets

Changara District, Mozambique, in October 2021 during durability monitoring data collection. Durability monitoring measures the physical condition and effectiveness of the chemicals on bed nets over time. Photo: PATH/Molly Robertson.
In December, the New Nets Project released its first interim report highlighting findings from five observational studies evaluating the effectiveness of insecticide-treated bed nets (ITNs) with new active ingredients. The studies use cross-sectional surveys, health system data, durability monitoring, mosquito surveillance, and anthropological inquiry to assess how these new nets perform in real-world implementation scenarios. Interim results show that ITNs remain one of our best tools to prevent malaria, and ITNs with new active ingredients seem to be better at reducing malaria in areas where mosquitos have developed resistance to the insecticides used on standard ITNs. This report includes only preliminary results. When results are finalized in 2022, they will help malaria program directors and the global community make decisions about which ITNs are more cost-effective in different settings.
The New Nets Project is funded by Unitaid and the Global Fund and led by IVCC. PATH, in partnership with national malaria programs and research institutions in sub-Saharan Africa, leads the observational pilots.


