Dr. Lambert Mukendi is going for zero—zero cases of human African trypanosomiasis (HAT). More commonly known as “sleeping sickness,” HAT is a neglected tropical disease that can cause neurological damage or even death if left untreated.
Lambert is part of a small team within Democratic Republic of the Congo’s (DRC's) Ministry of Health in charge of finding and confirming the few remaining cases of HAT. The country—once home to more than 80 percent of the world’s HAT cases—has committed to eliminating the disease by 2030.
Today, fewer than 400 detected cases remain. But, as Lambert explains, one single case of HAT is enough to declare a region endemic. That’s why his surveillance team is so critical to the elimination effort.
“We know from the history of this disease that when we relax, cases begin to rise again. We need to keep up the momentum through surveillance, vector control, and treatment.”
The strategy to eliminate HAT relies on persistent surveillance efforts, such as those led by Dr. Mukendi.
Training HAT experts
Dr. Lambert Mukendi is one of five scholars from the first cohort of the Victor Kande HAT Fellowship Program, a unique postgraduate program supported by the Bill & Melinda Gates Foundation and implemented by PATH in the DRC.
Named for the renowned Congolese doctor whose international work against HAT earned him the title "the father of sleeping sickness"—the Victor Kande HAT Fellowship Program supports in-depth studies in the field of public health.

Dr. Victor Kande gives remarks at a National HAT Day ceremony in Kinshasa where the fellowship was announced. Dr. Kande has spent more than 40 years of his life working to eliminate HAT. Photo taken pre-COVID-19: PATH/Sylvain Baloji.
Each year, twenty-five fellows from the DRC Ministry of Health receive additional training at the public health school of the University of Kinshasa in exchange for a minimum of two years of service to the DRC’s national sleeping sickness program, called Programme National de Lutte Contre la Trypanosomiase Humaine Africaine (PNLTHA).
Lambert did not always work on the forefront of HAT elimination. In 2007, he was a blood transfusion specialist at a clinic in Kasai Province when he signed on to a study that sought to identify if sleeping sickness could be contracted via human blood. He soon learned that this disease, which he had never heard of before, was actually one of the most neglected and fatal in the world.
His time working on the study piqued his interest in HAT. Following the study’s completion, Lambert moved to Kinshasa to work full-time for PNLTHA. In 2018, he learned about the Victor Kande Fellowship opportunity and eagerly applied.
During his time at the public health school in Kinshasa, Lambert says he learned about everything from computer science to epidemiology to project management. Throughout the one-year program, he was also sent on three different field visits to put his newly acquired skills to practice.
“My life changed completely,” says Lambert. “I now have new skills, am aware of new tools, and know how to manage an organizational structure.”
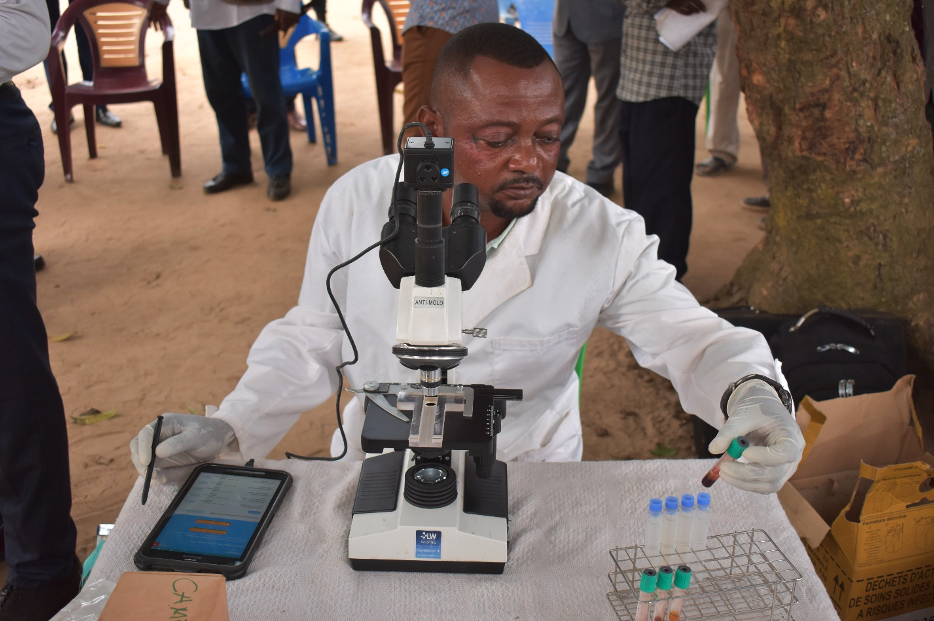
At any one time, dozens of mobile teams from the DRC Ministry of Health are deployed to villages around the country to test for human African trypanosomiasis (commonly known as sleeping sickness). Photo taken pre-COVID-19: PATH/Cassie Kobrin.
A bright future ahead
Since completing his studies, Dr. Lambert Mukendi has taken on greater responsibilities at PNLTHA. Today, he leads a surveillance team working to identify villages where HAT remains endemic.
Of the fellowship, he says he will always be thankful: “In the past, I could only talk about the health areas in which I worked. Now I am able to contribute to a broader range of public health discussions because I am more equipped with knowledge and competencies to do so.”



